Introducing EvoDASH: The Dashboard That Shows You What Your Lab Is Actually Doing
We have been building toward this for a while. Today, we are proud to announce the official launch of EvoDASH, the real-time lab performance dashboard built directly
Three Signs Your Lab’s Customer Relationships Are Running on Memory
If someone called your lab asking about a complaint from two months ago, how long would it take your team to piece together what happened? Not a
Atlanta Based Systems and Lighthouse Precision Case Tracking Light Up LMT LAB DAY Chicago 2026
48 years of dental lab software leadership met the future of case tracking at LMT LAB DAY Chicago. Read how the exclusive Evolution and Lighthouse integration stole
Join ABS at LMT Lab Day 2026: Booth H-13 Awaits with a Game-Changing Surprise!
Join ABS at Booth H-13 for LMT LAB DAY 2026 in Chicago on February 20th and 21st where we will be introducing a surprise guest integration!
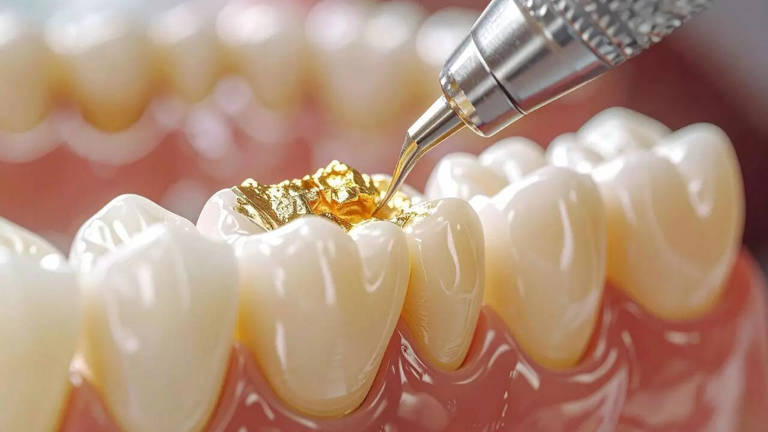
Revolutionizing Enamel Repair: Emerging Biomaterials Like Protein Gels and Zinc Compounds
Recent research on protein-based gels and zinc-containing compounds—often synergized with fluoride—is opening doors to non-invasive repairs that could eliminate the need for traditional fillings.
Revolutionize Your Dental Lab with Evolution’s New iTero Integration
Evolution Dental Lab Management Software now integrates seamlessly with iTero™ digital scanners, taking your lab’s workflow to new heights.